Flubromazepam

Fatal overdose may occur when benzodiazepines are combined with other depressants such as opiates, barbiturates, gabapentinoids, thienodiazepines, alcohol or other GABAergic substances.[1]
It is strongly discouraged to combine these substances, particularly in common to heavy doses.
| Summary sheet: Flubromazepam |
| Flubromazepam | |||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Chemical Nomenclature | |||||||||||||||||||||||||||
| Common names | Flubromazepam | ||||||||||||||||||||||||||
| Systematic name | 7-Bromo-5-(2-fluorophenyl)-1,3-dihydro-1,4-benzodiazepin-2-one | ||||||||||||||||||||||||||
| Class Membership | |||||||||||||||||||||||||||
| Psychoactive class | Depressant | ||||||||||||||||||||||||||
| Chemical class | Benzodiazepine | ||||||||||||||||||||||||||
| Routes of Administration | |||||||||||||||||||||||||||
|
|||||||||||||||||||||||||||
| Interactions | |||||||||||||||||||||||||||
Flubromazepam is a long-lasting psychoactive substance of the benzodiazepine class which produces anxiolytic, sedative, muscle relaxant, depressant and amnesic effects.
This compound was first made in 1960,[2] but was never marketed and did not receive any further attention or study until late 2012. It has potential use for the short-term treatment of anxiety, insomnia, acute seizures, and the sedation of hospitalized patients. However, it is currently exclusively sold by online research chemical vendors for use as a recreational psychoactive substance and has not been formally studied. This means that any comments regarding its pharmacology are purely speculation based upon the subjective effects it induces and its structural similarity to triazolam, pyrazolam and other benzodiazepines.
It's worth noting that the sudden discontinuation of benzodiazepines can be potentially dangerous or life-threatening for individuals regularly using for extended periods of time, sometimes resulting in seizures or death.[3] It is highly recommended to taper one's dose by gradually lowering the amount taken each day for a prolonged period instead of stopping abruptly.[4]
Chemistry
Flubromazepam, or 7-Bromo-5-(2-fluorophenyl)-1,3-dihydro-1,4-benzodiazepin-2-one, is a chemical of the benzodiazepine class. Flubromazepam is named for the fluorine and bromine substitutions on its core benzodiazepine skeleton (FLUorine-BROMine-azepam). Flubromazepam is a member of the benzodiazepine class as it contains a 1,4 diazepine ring fused to a substituted benzene ring. Bromine is bound to this bicyclic structure at R7. Additionally, a fluorine-substituted phenyl ring is bound to this structure at R5. Flubromazepam also contains an oxygen group double bonded to R2 of its diazepine ring to form a ketone. This oxygen substitution at R2 is shared with other benzodiazepine drugs with the suffix -azepam.
Pharmacology
Flubromazepam has turned out to be a hazardous yet valuable medication for humankind since it can be utilized as a painkiller. Flubromazepam can ease that pain as it has muscle-relaxing effects. The exact pharmacological activity of Flubromazepam are not confirmed by verified data, but existing studies seem to suggest certain amounts anxiolytic, sedative, and muscle-relaxing potential.
Benzodiazepines produce a variety of effects by binding to the benzodiazepine receptor site and magnifying the efficiency and effects of the neurotransmitter gamma aminobutyric acid (GABA) by acting on its receptors.[5] As this site is the most prolific inhibitory receptor set within the brain, its modulation results in the sedating (or calming effects) of flubromazepam on the nervous system.
The anticonvulsant properties of benzodiazepines may be, in part or entirely, due to binding to voltage-dependent sodium channels rather than benzodiazepine receptors.[6]
Subjective effects
Disclaimer: The effects listed below cite the Subjective Effect Index (SEI), an open research literature based on anecdotal user reports and the personal analyses of PsychonautWiki contributors. As a result, they should be viewed with a healthy degree of skepticism.
It is also worth noting that these effects will not necessarily occur in a predictable or reliable manner, although higher doses are more liable to induce the full spectrum of effects. Likewise, adverse effects become increasingly likely with higher doses and may include addiction, severe injury, or death ☠.
Physical effects 
-
- Sedation - In terms of energy level alterations, this substance has the potential to become very sedating in a rapid-acting fashion. At higher doses, this can lead users to suddenly feel as if they are extremely sleep deprived and have not slept for days, forcing them to sit down and generally feel as if they are constantly on the verge of passing out. This sense of sleep deprivation increases proportional to dosage and eventually becomes powerful enough to force a person into complete unconsciousness.
- Muscle relaxation
- Physical euphoria
- Motor control loss
- Respiratory depression
- Increased libido
- Seizure suppression[citation needed]
- Appetite enhancement - This effect is not particularly prominent, but is reported to occur in some people. It can have a synergistic effect when combined with cannabis.
- Dizziness
- Temporary erectile dysfunction
Paradoxical effects 
-
Paradoxical reactions to benzodiazepines such as increased seizures (in epileptics), aggression, increased anxiety, violent behavior, loss of impulse control, irritability and suicidal behavior sometimes occur (although they are rare in the general population, with an incidence rate below 1%).[7][8]
These paradoxical effects occur with greater frequency in recreational abusers, individuals with mental disorders, children, and patients on high-dosage regimes.[9][10]
Cognitive effects 
-
- Anxiety suppression
- Disinhibition
- Cognitive euphoria - This effect is generally produced only at high doses, and is thought to arise largely from the release of pre-existing anxiety in the user. Many users report not feeling any pleasurable or euphoric sensations from benzodiazepines at all.
- Compulsive redosing - This component is likely due to the rapid way in which the substance produces its anxiety-relieving, relaxing and sometimes euphoric effects before quickly dropping off. It can be made worse due to the memory suppression it produces which can lead the user forgetting they have taken any at all, which can lead to a cycle that leads to a dangerous amnesic blackout state.
- Memory suppression
- Delusions of sobriety - This is the false belief that one is perfectly sober despite obvious evidence to the contrary such as severe cognitive impairment and an inability to fully communicate with others. It most commonly occurs at high to heavy dosages.
- Analysis suppression
- Ego inflation
- Thought deceleration
- Motivation suppression
- Emotionality suppression - Although this compound primarily suppresses anxiety, it also dulls other emotions in a manner which is distinct but less intensive than that of antipsychotics.
- Sleepiness
After effects 
-
- Rebound anxiety - Rebound anxiety is a commonly observed effect with anxiety relieving substances like benzodiazepines. It typically corresponds to the total duration spent under the substance's influence along with the total amount consumed in a given period, an effect which can easily lend itself to cycles of dependence and addiction.
- Dream potentiation or Dream suppression
- Residual sleepiness
- Thought deceleration
- Thought disorganization
- Irritability
Experience reports
There are currently no anecdotal reports which describe the effects of this compound within our experience index. Additional experience reports can be found here:
Toxicity and harm potential
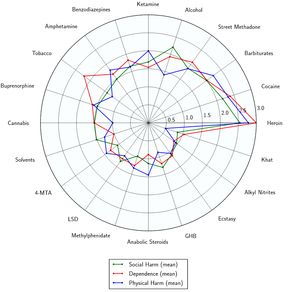
Flubromazepam likely has a low toxicity relative to dose.[12] However, it is potentially lethal when mixed with depressants like alcohol or opioids.
It is strongly recommended that one use harm reduction practices when using this drug.
Tolerance and addiction potential
Flubromazepam is extremely physically and psychologically addictive.
Tolerance will develop to the sedative-hypnotic effects within a couple of days of continuous use. After cessation, the tolerance returns to baseline in 7 - 14 days. However, in certain cases, this may take significantly longer in a manner which is proportional to the duration and intensity of one's long-term usage.
Withdrawal symptoms or rebound symptoms may occur after ceasing usage abruptly following a few weeks or longer of steady dosing and may necessitate a gradual dose reduction. For more information on tapering from benzodiazepines in a controlled manner, please see this guide.
Benzodiazepine discontinuation is notoriously difficult; it is potentially life-threatening for individuals regularly using to discontinue use without tapering their dose over a period of weeks. There is an increased risk of hypertension, seizures, and death.[3] Drugs which lower the seizure threshold such as tramadol should be avoided during withdrawal.
Flubromazepam presents cross-tolerance with all benzodiazepines, meaning that after its consumption, all benzodiazepines will have a reduced effect.
Dangerous interactions
Although many drugs are safe on their own, they can become dangerous and even life-threatening when combined with other substances. The list below contains some common potentially dangerous combinations, but may not include all of them. Certain combinations may be safe in small doses of each but still, increase the potential risk of death. Independent research should always be done to ensure that a combination of two or more substances is safe before consumption.
- Depressants (1,4-Butanediol, 2-methyl-2-butanol, alcohol, barbiturates, GHB/GBL, methaqualone, opioids) - This combination can result in dangerous or even fatal levels of respiratory depression. These substances potentiate the muscle relaxation, sedation and amnesia caused by one another and can lead to unexpected loss of consciousness at high doses. There is also an increased risk of vomiting during unconsciousness and death from the resulting suffocation. If this occurs, users should attempt to fall asleep in the recovery position or have a friend move them into it.
- Dissociatives - This combination can result in an increased risk of vomiting during unconsciousness and death from the resulting suffocation. If this occurs, users should attempt to fall asleep in the recovery position or have a friend move them into it.
- Stimulants - It is dangerous to combine benzodiazepines with stimulants due to the risk of excessive intoxication. Stimulants decrease the sedative effect of benzodiazepines, which is the main factor most people consider when determining their level of intoxication. Once the stimulant wears off, the effects of benzodiazepines will be significantly increased, leading to intensified disinhibition as well as other effects. If combined, one should strictly limit themselves to only dosing a certain amount of benzodiazepines per hour. This combination can also potentially result in severe dehydration if hydration is not monitored.
Overdose
Benzodiazepine overdose may occur when a benzodiazepine is taken in large quantities or concurrently with other depressants. This is particularly dangerous with other GABAergic depressants such as barbiturates and alcohol since they work similarly, but bind to distinct allosteric sites on the GABAA receptor. Thus their effects potentiate one another. Benzodiazepines increase the frequency in which the chlorine ion pore opens on the GABAA receptor while barbiturates increase the duration in which they are open, meaning when both are consumed, the ion pore will open more frequently and stay open longer[13]. Benzodiazepine overdose is a medical emergency that may lead to a coma, permanent brain injury or death if not treated promptly and appropriately.
Symptoms of a benzodiazepine overdose may include severe thought deceleration, slurred speech, confusion, delusions, respiratory depression, coma or death. Benzodiazepine overdoses may be treated effectively in a hospital environment, with generally favorable outcomes. Benzodiazepine overdoses are sometimes treated with flumazenil, a GABAA antagonist[14]. However, care is primarily supportive in nature.
Legal status
 |
This legality section is a stub. As such, it may contain incomplete or wrong information. You can help by expanding it. |
- Canada: All benzodiazepines are listed in Schedule IV.[15]
- Germany: Flubromazepam is controlled under Anlage II BtMG (Narcotics Act, Schedule II)[16] as of November 21, 2015.[17] It is illegal to manufacture, possess, import, export, buy, sell, procure or dispense it without a license.[18]
- Russia: Flubromazepam is a Schedule III controlled substance since 2017.[19]
- Switzerland: Flubromazepam is a controlled substance specifically named under Verzeichnis E.[20]
- Turkey: Flubromazepam is a classed as drug and is illegal to possess, produce, supply, or import.[21]
- United Kingdom: Flubromazepam is a Class C controlled substance as of May 31, 2017. It is illegal to possess, produce or supply.[22]
- United States: Flubromazepam is Schedule 1 controlled substance under Virginia State law, but is not federally scheduled.[23]
Preparation methods
- Volumetric liquid dosing - If the benzodiazepine is in a powder form, it is unlikely to weigh out accurately without the most expensive of scales due to its activity in such small amounts. To avoid this, one can dissolve the benzodiazepine volumetrically into a solution and dose it accurately based upon the methodological instructions linked within this tutorial here.
See also
External links
References
- ↑ Risks of Combining Depressants - TripSit
- ↑ Earl, R., Henryk, S. L., Amino substituted benzophenone oximes and derivatives thereof
- ↑ 3.0 3.1 Lann, M. A., Molina, D. K. (June 2009). "A fatal case of benzodiazepine withdrawal". The American Journal of Forensic Medicine and Pathology. 30 (2): 177–179. doi:10.1097/PAF.0b013e3181875aa0. ISSN 1533-404X.
- ↑ Kahan, M., Wilson, L., Mailis-Gagnon, A., Srivastava, A. (November 2011). "Canadian guideline for safe and effective use of opioids for chronic noncancer pain. Appendix B-6: Benzodiazepine Tapering". Canadian Family Physician. 57 (11): 1269–1276. ISSN 0008-350X.
- ↑ Haefely, W. (29 June 1984). "Benzodiazepine interactions with GABA receptors". Neuroscience Letters. 47 (3): 201–206. doi:10.1016/0304-3940(84)90514-7. ISSN 0304-3940.
- ↑ McLean, M. J., Macdonald, R. L. (February 1988). "Benzodiazepines, but not beta carbolines, limit high frequency repetitive firing of action potentials of spinal cord neurons in cell culture". The Journal of Pharmacology and Experimental Therapeutics. 244 (2): 789–795. ISSN 0022-3565.
- ↑ Saïas, T., Gallarda, T. (September 2008). "Paradoxical aggressive reactions to benzodiazepine use: a review". L’Encephale. 34 (4): 330–336. doi:10.1016/j.encep.2007.05.005. ISSN 0013-7006.
- ↑ Paton, C. (December 2002). "Benzodiazepines and disinhibition: a review". Psychiatric Bulletin. 26 (12): 460–462. doi:10.1192/pb.26.12.460. ISSN 0955-6036.
- ↑ Bond, A. J. (1 January 1998). "Drug- Induced Behavioural Disinhibition". CNS Drugs. 9 (1): 41–57. doi:10.2165/00023210-199809010-00005. ISSN 1179-1934.
- ↑ Drummer, O. H. (February 2002). "Benzodiazepines - Effects on Human Performance and Behavior". Forensic Science Review. 14 (1–2): 1–14. ISSN 1042-7201.
- ↑ Nutt, D., King, L. A., Saulsbury, W., Blakemore, C. (24 March 2007). "Development of a rational scale to assess the harm of drugs of potential misuse". The Lancet. 369 (9566): 1047–1053. doi:10.1016/S0140-6736(07)60464-4. ISSN 0140-6736.
- ↑ Mandrioli, R., Mercolini, L., Raggi, M. A. (October 2008). "Benzodiazepine metabolism: an analytical perspective". Current Drug Metabolism. 9 (8): 827–844. doi:10.2174/138920008786049258. ISSN 1389-2002.
- ↑ Twyman, R. E., Rogers, C. J., Macdonald, R. L. (March 1989). "Differential regulation of gamma-aminobutyric acid receptor channels by diazepam and phenobarbital". Annals of Neurology. 25 (3): 213–220. doi:10.1002/ana.410250302. ISSN 0364-5134.
- ↑ Hoffman, E. J., Warren, E. W. (September 1993). "Flumazenil: a benzodiazepine antagonist". Clinical Pharmacy. 12 (9): 641–656; quiz 699–701. ISSN 0278-2677.
- ↑ Branch, L. S. (2022), Consolidated federal laws of Canada, Controlled Drugs and Substances Act
- ↑ "Anlage II BtMG" (in German). Bundesministerium der Justiz und für Verbraucherschutz. Retrieved December 19, 2019.
- ↑ "Dreißigste Verordnung zur Änderung betäubungsmittelrechtlicher Vorschriften" (PDF). Bundesgesetzblatt Jahrgang 2015 Teil I. Nr. 45 (in German). Bundesanzeiger Verlag. November 20, 2015. Retrieved December 29, 2019.
- ↑ "§ 29 BtMG" (in German). Bundesministerium der Justiz und für Verbraucherschutz. Retrieved December 19, 2019.
- ↑ Постановление Правительства РФ от 12.07.2017 N 827 “О внесении изменений в некоторые акты Правительства Российской Федерации в связи с совершенствованием контроля за оборотом наркотических средств и психотропных веществ” - КонсультантПлюс
- ↑ "Verordnung des EDI über die Verzeichnisse der Betäubungsmittel, psychotropen Stoffe, Vorläuferstoffe und Hilfschemikalien" (in German). Bundeskanzlei [Federal Chancellery of Switzerland]. Retrieved January 1, 2020.
- ↑ https://resmigazete.gov.tr/eskiler/2017/01/20170112-8.pdf
- ↑ The Misuse of Drugs Act 1971 (Amendment) Order 2017
- ↑ 18VAC110-20-322. Placement of chemicals in Schedule I.